Subtotal $0.00
Subscribe to out newsletter today to receive latest news administrate cost effective for tactical data.
717 Lee Street, Apt 8 Mesquite, TX 75149, United States
Subscribe to out newsletter today to receive latest news administrate cost effective for tactical data.
717 Lee Street, Apt 8 Mesquite, TX 75149, United States
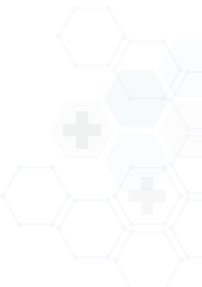
Our denial management services minimize claim denials and expedite payments, boosting your cash flow and reducing financial strain. This allows you to focus on providing exceptional care, knowing your reimbursements are handled promptly and accurately.

Our team is constantly updated with the latest coding practices, payer guidelines, and regulatory requirements. We bring extensive experience in ICD-10, CPT, and HCPCS codes, ensuring full compliance and reducing the risk of costly errors.

Whether you're a small practice or a large healthcare organization, we tailor our services to your needs. We specialize in fields including radiology, cardiology, orthopedics, and more—adapting our approach to your size and challenges to ensure maximum benefit.
You Get Our More services... Explore All Service
01
Accurate collection of patient demographics and insurance information to ensure clean claim generation from the outset. Ensures 100% accuracy in patient demographic capture.

02
Real-time validation of coverage, benefits, and authorization requirements to minimize rejections and billing delays. Helps reduce claim denials by up to 40% through proactive eligibility verification.
03
Conversion of clinical notes into compliant CPT, ICD-10, and HCPCS codes—ensuring payer accuracy and revenue integrity. Achieves 98% coding accuracy with certified coding specialists.

04
Systematic entry of billable services aligned with payer guidelines and charge master, enabling proper claim valuation. Accelerates claim readiness within 24 hours.

05
Automated submission of claims to payers through integrated clearinghouses, reducing turnaround time and error rates. Achieves a 99% clean claim rate through automation.

06
Insurance carriers evaluate claims for benefit eligibility, medical necessity, and coding accuracy before reimbursement.

07
Accurate application of payer remittances and patient payments to account balances, enabling real-time revenue tracking. Posts payments within 48 hours to ensure up-to-date financials.

08
Targeted follow-up on denied or underpaid claims using root-cause analysis and structured appeal strategies. Recovers up to 90% of denied claims through effective appeals.

09
Professional generation of patient statements and execution of ethical collection strategies to resolve outstanding balances. Improves patient payment rates by up to 25% through clear communication and flexible options.

10
Comprehensive insights into revenue cycle performance using KPI dashboards and audit-ready financial reporting. Provides actionable insights with real-time dashboards to optimize revenue.

• 20% Faster Payments: On average, our clients experience 20% faster payments after partnering with us, helping to accelerate their cash flow.

• 30% Reduction in Claim Denials: By addressing the root causes of denials and improving the accuracy of claims, our clients typically see a 30% reduction in claim denials within the first 6 months of working with us.