Subtotal $0.00
Subscribe to out newsletter today to receive latest news administrate cost effective for tactical data.
717 Lee Street, Apt 8 Mesquite, TX 75149, United States
Subscribe to out newsletter today to receive latest news administrate cost effective for tactical data.
717 Lee Street, Apt 8 Mesquite, TX 75149, United States
01
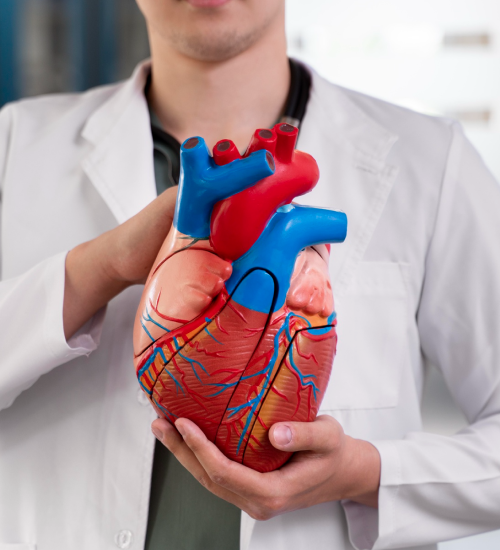
We gather and verify all required documentation: o Medical licenses & board certifications.... o Work & education history............. o Malpractice coverage.................... o References & hospital privileges

02
We submit complete, payer-ready applications to minimize rejections and speed up processing.
03
Insurance companies validate credentials with issuing institutions—education, licensure, and employment.

04
We proactively resolve application gaps or missing information to avoid unnecessary delays.

05
We manage communication and follow-ups with payers to ensure applications move smoothly.

06
For in-network status, we assist with contract negotiation and agreement reviews.

07
Regular updates for licenses, insurance, and credentials to keep your profile active and compliant.
• 20% Faster Payments: On average, our clients experience 20% faster payments after partnering with us, helping to accelerate their cash flow.

• 30% Reduction in Claim Denials: By addressing the root causes of denials and improving the accuracy of claims, our clients typically see a 30% reduction in claim denials within the first 6 months of working with us.